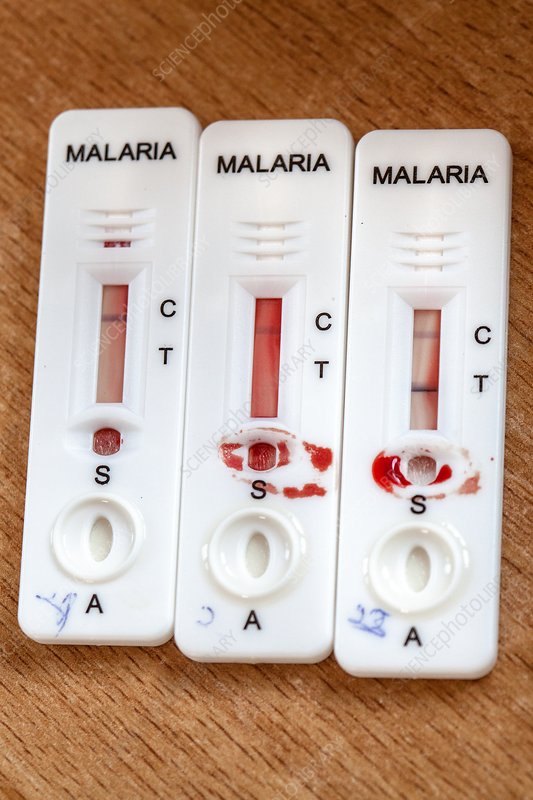
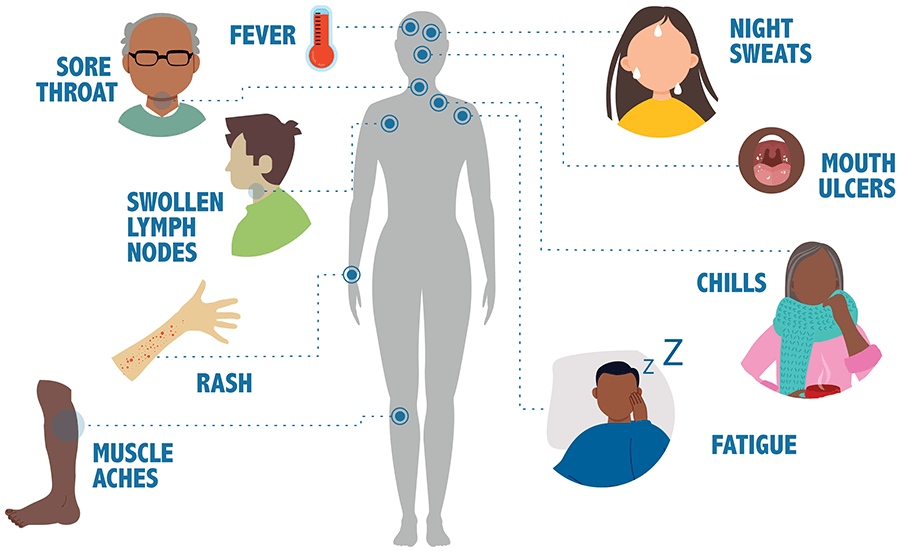
My curiosity made me to find out what keeps us moving in this world but to my surprise, it was revealed that there are three key foundations a country stands on; Health, Education and Agriculture. Each of these is interdependent. We need knowledge to understand our health, and we need food to give us energy to be able to acquire knowledge and stay healthy. With this, it can be argued that any smart nation or individual must invest in Health, Education, and Agriculture. This leads us to our discussion on health investment and how smart it should be!
According to World Health Organisation (WHO): “Health is a human right”, hence everyone has right to good health but this is not achieved on a silver platter, it takes a lot of work and planning as individual, institutions and government at large to achieve this. With proper planning, you can easily have good health to enjoy the world flexibly and freely. Https:www.nuviewnutrition.com asserted that “make health a lifestyle rather than a chore”. This means it is very wise to invest in the food we eat mundane, activities of daily living like exercises, managing our stresses, making more time for our body, mind and soul, our sexual life as well as spiritual life. This reminded me of my favourite quote I love so much from Heather Morgan that “every time you eat or drink, you are either feeding disease or fighting it”.
Additionally, from my personal experiences as a nurse clinician, it is very regrettable and extremely sad that sometimes money cannot buy health when very wealthy people are in sick beds. Some of my encounters revealed most rich people were busy chasing wealth than their health, and by the time ‘they’ obtained the wealth, their health are at deteriorating stage where nothing can be done. In a nutshell, be smart to invest in your health too as you chase the wealth so that you can enjoy your wealth in a healthy state. What gains do you get if you chase all the wealths in the world, neglecting your health consciously or unconsciously then someone who did not ‘sweat some’ enjoys the wealth when you’re terminally ill or dead?
To The Institutions and Government………….
According to WHO’s article titled “Health is a smart investment”, any nation with a good primary health care makes the population healthier. It was also noted in this article that most money goes into healthcare provided in hospitals rather than primary health care. Another revelation was that “the first line of defence against outbreaks and health emergencies is Primary Health Care”. For us to understand and appreciate the arguments made by WHO, we need to understand the Primary Health Care and its concept, hence, the next discussion.
WHO described Primary Health Care as “A comprehensive healthcare centred on the needs and preferences of individuals, families and communities throughout the lifespan, not just for a set of specific diseases”. In simple term; screening and treating common diseases, providing promotive and preventive health care like vaccinations, health information for behaviour change. WHO argued that Strong Primary Health Care system saves money for the state. For instance, people across the length and breadth of the country need to journey costly to hospitals where healthcare is more expensive to provide. The cost in caring for one with terminal illness can make the whole family wheel in a cycle of poverty. This can make one to make a decision between his or her mother’s medications and his or her child’s education which should not be so. Investing in Primary Health Care helps to obtain healthy productive populations to drive the economic growth. And this saves money for the state.
WHO estimates one trillion US dollars investment in health by 2030 if prevention and control efforts are not taking very serious. Ministry of Health (MOH) document titled Health financing in Ghana sighted revealed that by 2030, our population will increase by almost 40% and older 65 and above will increase by 90% which will burden our health financial needs or escalate our Total Health Expenditure (THE). It is therefore critical for government to invest in population control using health information strategies as one of the pillars of Primary Health Care to sensitise the public.
Health Expenditure…………
For you to appreciate smart health investment, it is only logical to discuss briefly health expenditure. Health expenditure in short is health spending. Let’s have in mind the two key terms which will be used in the discussions; Government health spending (health bills covered by national health insurance) and Out-of-pocket health spending ( health bills not covered by national health insurance and are paid directly by the private or individual.
Taking a critical look at the WHO Global Health Expenditure chart below of some selected countries like Ghana, the United Kingdom, the United States, and South Africa; Ghana our beloved country is not doing badly at all in government health spending, and reducing the out-of-pocket health spending to lower health financial burden on individuals, but there is more room for improvement.
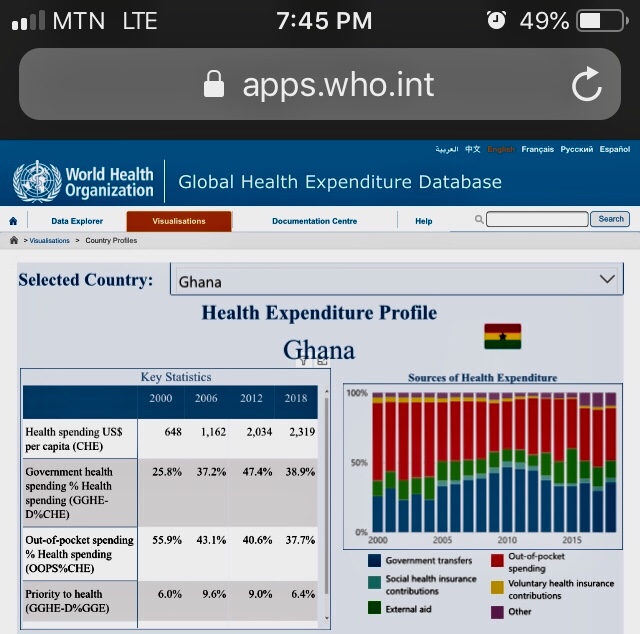
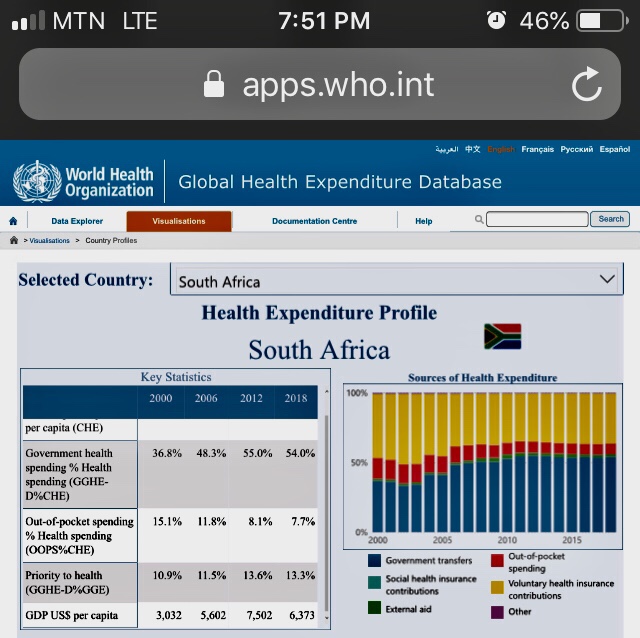
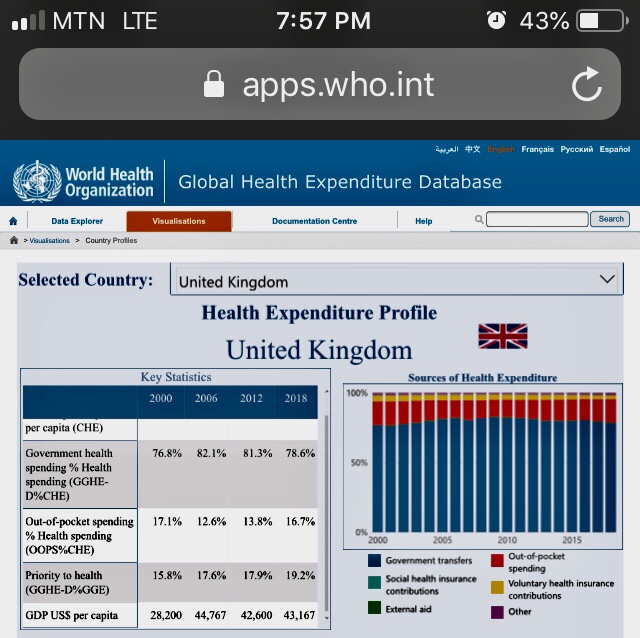
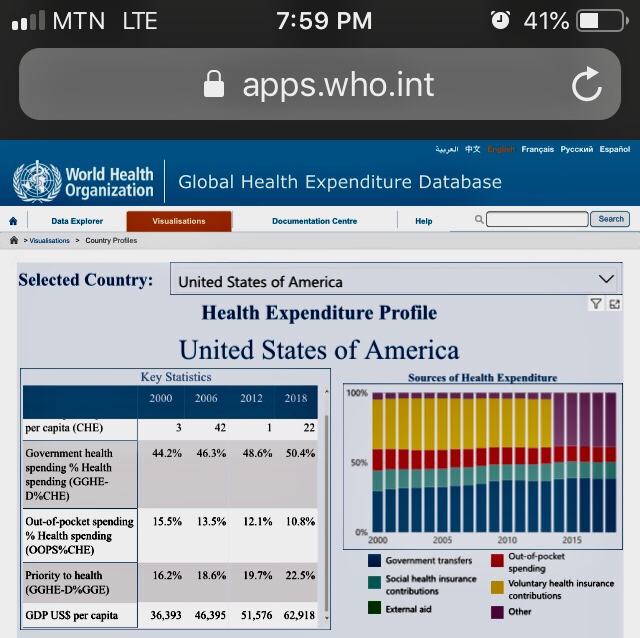
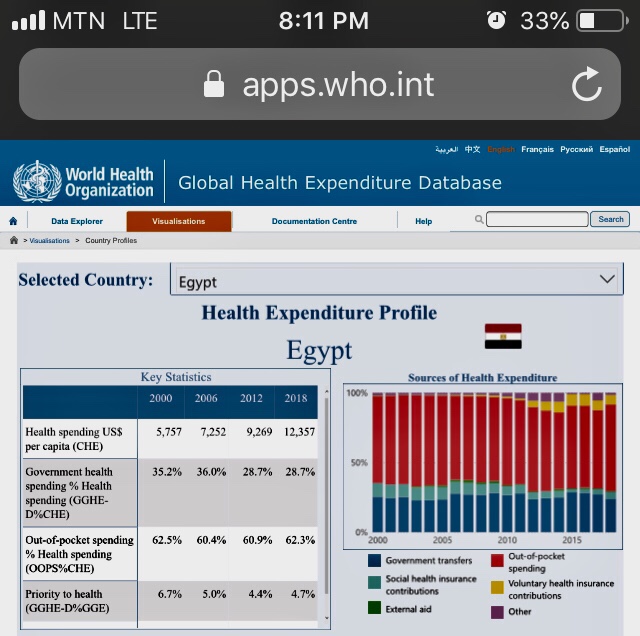
In conclusion, we as individuals should invest smartly in our personal health, paying attention to our promotive and preventative health as we chase the wealth. We should let our health be our lifestyle, not chore. To the institutions and government, let us invest most of the health spending into Primary Health Care to save the nation; let’s change the common mindset that investment in health is investment in hospitals. Let’s celebrate the new year safely by observing all the safety protocols because new variants of COVID-19 is aggressively emerging .
Sources: